Please help contribute to research by answering this brief survey about chronic pain
Your responses will help us conduct research to serve patients better.
If you read our first post on “what is chronic pain”, you’ll know that pain catastrophizing, fear of movement, anxiety, and nervous system sensitization are the main drivers of pain and disability in those that have chronic musculoskeletal pain. Naturally, it is these factors that must be addressed for us to embark on the road to recovery (Booth et al., 2017).
High level evidence suggests that nonpharmacological approaches such as physiotherapy, counselling, and self-management strategies should be the first line treatment for all people with chronic pain (Dynamed, 2022). You can decide what approaches are best for you in collaboration with your doctor and health care team.
How Physiotherapy and Exercise Can Help Chronic Pain
There are three ways that physiotherapy and exercise improve pain and disability with those that have chronic pain: physical changes; psychological effects; and neurophysiological effects
1. Physical changes: there are many physiological changes that occur when we exercise over a long period of time. Depending on the type of exercise, these include increased muscular endurance, increased strength, and increased range of motion. However, the evidence on these physical changes leading to decreased pain is less clear. Part of this is because research has found that the pain-relieving effects of exercise are non-specific. That is, it doesn’t matter what type of exercise you do, your pain will decrease! This is because it has less to do with you getting big muscles and being super flexible and more to do with the psychological and neurophysiological effects of exercise (Booth et al., 2017).
2. Psychological effects: exercise can and does reduce anxiety, fear of movement, and pain catastrophization while boosting self-efficacy—all of which have the ability to reduce pain (Booth, 2017). However, the catch 22 is that if you have chronic pain, and you identify with some of these psychological factors, the thought of exercising can be daunting! If exercise or movement has caused you pain in the past, it is natural to have some fear associated with it. For this reason, you might consider working with a physiotherapist that can help you create a gradual exercise program. This will help to normalize exercise and teach your nervous system that movement is safe.
Research also shows that for people with chronic pain, exercise combined with pain neuroscience education (PNE) is more effective than exercise alone. PNE is a skill that physiotherapists are trained in that helps people to shift their perception from pain being evidence of tissue damage to persistent pain being related to an overactive protection response from the nervous system. In other words, learning that hurt does not equal harm, and that pain is not evidence of tissue damage, can both reduce your pain and empower you to exercise (Booth et al., 2017; Watson et al., 2019).
3. Neurophysiological effects: exercise-induced analgesia and functional and structural changes in the brain (thanks to exercise) reduce pain. Exercise-induced analgesia is a fancy term that means exercise can have pain relieving effects similar to medications—it’s just that instead of getting something from the pharmacy, you’re hacking your body’s built-in pharmacological system. There are many chemicals within our nervous system that exercise can release, such as endogenous opioids, nitric oxide, catecholamines, endocannabinoids, and serotonin, all of which can and do modulate pain perception (Da Silva Santos & Galdino, 2018).
How to Exercise With Chronic Pain (Without Flare-Ups)
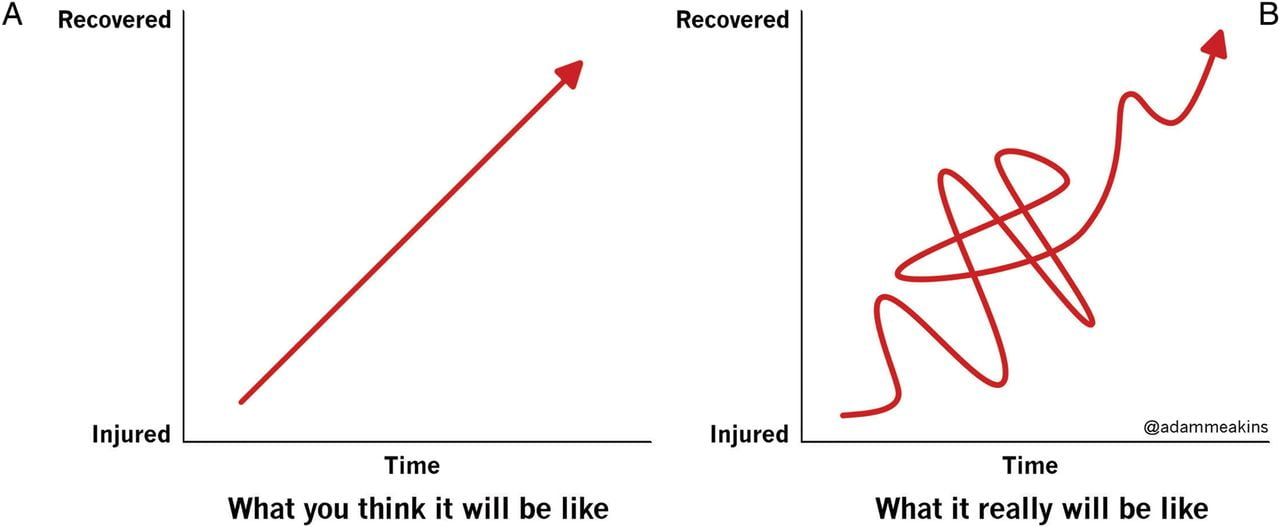
All the benefits of exercise are great, but you might be asking yourself, what if exercising causes a pain flare up? The truth is it might—and accepting that may help you to stick to exercise and other self-management strategies more long term. As much as we want it to be, healing is not linear, and we love Adam Meakins depiction of the healing journey below:
Pace Yourself
Many people with chronic pain will overdo it on the days that they’re feeling well, which leads to a boom-and-bust cycle. In other words, you might do a ton while you’re feeling well which could lead to a pain flare up in the days following. It is important that you respect your current capacity for exercise—and because we are not one-dimensional beings, our capacity will be impacted by many factors such as sleep, stress, nutrition, relationships, and mental well-being. For this reason, it’s important to accept that embarking on the healing journey may include flare ups and these may be better managed if you have a physiotherapist to assist you in pacing and exercise prescription.
Counselling
There is high level evidence that supports counselling as one of the first line treatments for chronic pain. This is especially true for counselling that focuses on behavioural interventions to address topics such as pain catastrophization; fear of activity and exercise; and sleep hygiene. Evidence suggests that cognitive behavioural therapy (CBT); acceptance and commitment therapy (ACT); mindfulness-based stress reduction (MBSR); and progressive relaxation are the most effective for chronic pain, so you might consider finding professionals that are trained in those techniques (NICE guidelines, 2021).
6 Chronic Pain Self-Management Strategies
Sleep disorders are reported in 50-88% of patients with chronic pain (Dynamed, 2022) so supporting better sleep may be a helpful tool. You can get support from your doctor or counsellor, and you can also consider the sleep hygiene practices below.
- Set up your environment to support sleep (ideal temperature, dark, quiet)
- Avoid going to bed until feeling drowsy and ready to sleep.
- Don’t watch the clock
- Get out of bed if not asleep in 15-20 minutes and return only when drowsy
- Avoid substances that interfere with sleep before bedtime (caffeine, alcohol, nicotine)
- Exercise regularly, at least 6 hours before sleep
(Schutte-Rodin, Broch, Buysee, Dorsey, & Sateia, 2008).
We hope that for those living with chronic pain, this quick overview on treatment approaches inspires hope. And remember, you don’t have to do this alone, and the help of a good team of health care professionals can make a world of difference (Lamper, Beckers, Kroese, Verbunt, Huijnen, 2021).
If you live on Vancouver Island and need help with chronic pain, visit us at Parkway Physiotherapy & Performance Centre.