The Parkway Physiotherapy Blog
-

How Neuroplasticity Works in Stroke Recovery: Rewiring the Brain
The idea that the brain can rebuild itself after a stroke once sounded impossible. Today, it is one of the most important principles guiding…
-

Parkinson’s Physiotherapy: Improving Mobility and Independence
Parkinson’s disease is a progressive neurological disorder that primarily affects the brain’s ability to produce dopamine. Dopamine is the chemical messenger responsible for coordinating…
-

Do All Meniscus Tears Require Surgery?
The sudden pop or twist in a knee followed by persistent aching and clicking often leads to an immediate fear that surgery is the…
-
Physiotherapy for Rotator Cuff Tendinopathy: What You Should Know Before You Try to “Push Through” the Pain
Lifting your arm to grab something from the cupboard shouldn’t feel like a negotiation. Neither should rolling onto your shoulder at night or reaching…
-
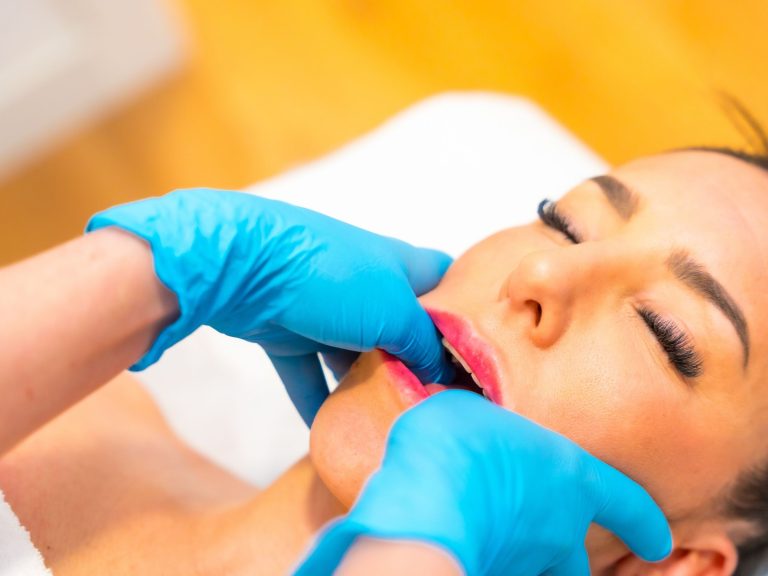
Jaw Pain Relief: How Specialized Physiotherapy Can Conquer Jaw Pain
Jaw pain is more than just an inconvenience; it can be a persistent, debilitating condition that impacts everything from eating and speaking to sleeping…
-
Growth Plate (Physeal) Injuries in Youth Climbers
Rachel Rubin-Sarganis MScPT | Physiotherapist | Parkway Physiotherapy Tuscany Village What Are Growth Plates? Growth plates are cartilage zones at the ends of long…
-
Lumbrical injuries in Climbers
Rachel Rubin-Sarganis MScPT | Physiotherapist | Parkway Physiotherapy Tuscany Village What Are Lumbrical Muscles? Each hand contains four lumbrical muscles, located in the deep…
-
TFCC Injuries in Climbers
Rachel Rubin-Sarganis MScPT | Physiotherapist | Parkway Physiotherapy Tuscany Village What Is the TFCC? The Triangular Fibrocartilage Complex (TFCC) is a group of structures…
-
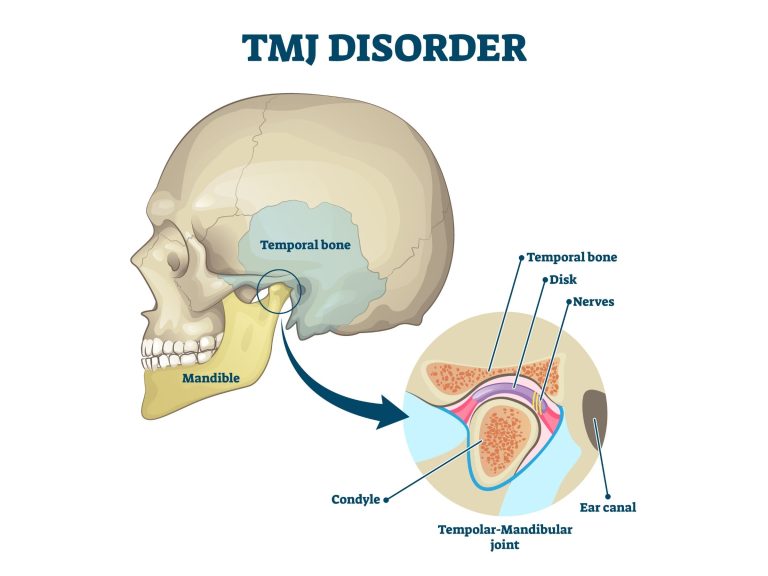
Clicking, Popping, or Locking? Reclaiming Your Jaw with Physiotherapy for Disc Displacement
That unsettling click, pop, or even a sudden “lock” in your jaw can be alarming. These symptoms are often signs of TMJ Disc Displacement,…
-
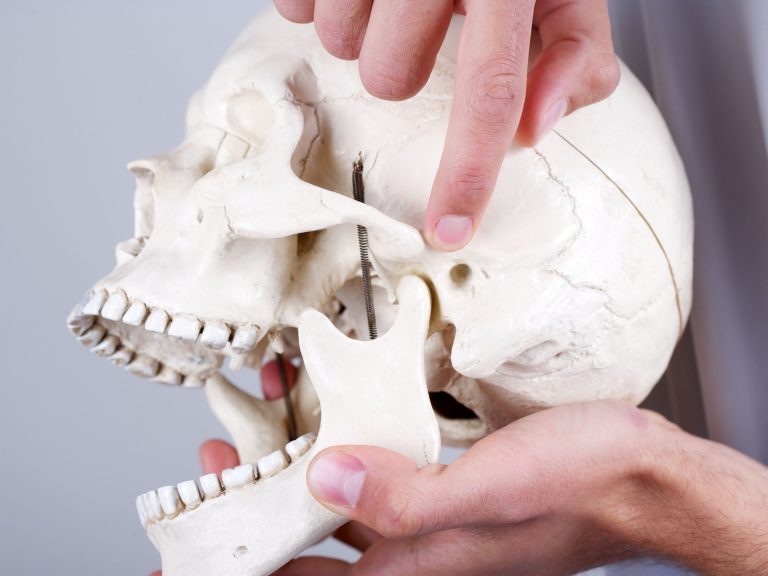
Taming the Overly Mobile Jaw: Physiotherapy for TMJ Hypermobility
Does your jaw sometimes feel like it moves too far? Do you experience frequent clicking, popping, or even a sensation of your jaw “getting…
-
Managing TMJ Arthritis: Finding Comfort and Function with Specialized Physiotherapy
Just like other joints in your body, your Temporomandibular Joint (TMJ, also known as the jaw) can be affected by arthritis, also known as…
-
TMJ Post-Surgical Recovery: A Physiotherapy Guide to Jaw Rehabilitation
If you’ve undergone TMJ surgery (such as arthroscopy or open-joint surgery), you’ve taken a significant step toward improving your jaw health. However, the procedure…
-
Finger Pulley Tears in Climbers
The fingers have a system of flexor tendons that run along their length, secured by strong ligament bands called pulleys. These pulleys keep the…
-
Shin Splints: Causes and Treatment for Langford Runners
If you’re a runner in Langford and Victoria’s Westshore, you may have experienced an aching pain along the front of your lower leg. This…
-
5 Effective Ways to Treat Achilles Tendinitis
Facing Achilles tendinitis can be painful and frustrating. Finding the right treatment is key to recovery and preventing future flare-ups. In this article, you’ll…
-
Addressing Incontinence with Pelvic Floor Physiotherapy
Dealing with incontinence can be challenging, but there are effective ways to manage it. Pelvic floor physiotherapy offers a promising approach to improve incontinence…
-
Contact with the Present Moment and Self-As-Context
How can we work with patients/clients who are easily distracted, disengaged, disconnected from thoughts and feelings, or appear stuck in the past or preoccupied…
-
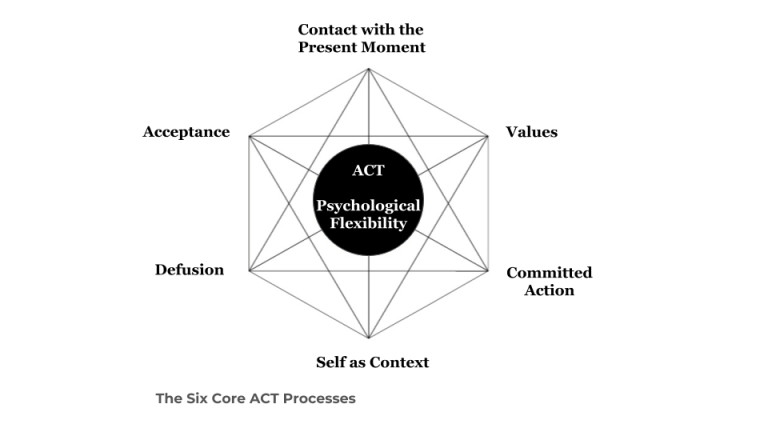
Acceptance and Commitment Therapy (ACT) in the Treatment of Pain
As a clinical counsellor, I am dedicated to individualized treatment, and I draw from and integrate different evidence-based approaches based on the client’s needs,…
-
Pelvic Floor Exercises for Postpartum Recovery
Discover effective pelvic floor exercises for postpartum recovery. Learn how to regain strength, improve bladder control, and support overall well-being after childbirth.
-
Comprehensive Guide to Pelvic Floor Physiotherapy
Learn everything you need to know about pelvic floor health in this comprehensive guide. Discover treatments, benefits, and how Parkway Physiotherapy can help you…